Stress, Sleep, and the “Hidden” Blood Sugar Spikes
At Primary Prevention Center PLLC in Newtown, PA, our team addresses how stress and poor sleep can lead to hidden blood sugar spikes that may go unnoticed. Stress triggers the release of cortisol, which can affect blood sugar levels, while inadequate sleep disrupts hormone balance, making it harder to manage glucose. We provide personalized strategies to manage stress, improve sleep quality, and stabilize blood sugar levels for better health. For more information, contact us or request an appointment online. We are located at 638 Newtown-Yardley Road Suite 2G/H, Newtown, PA 18940.
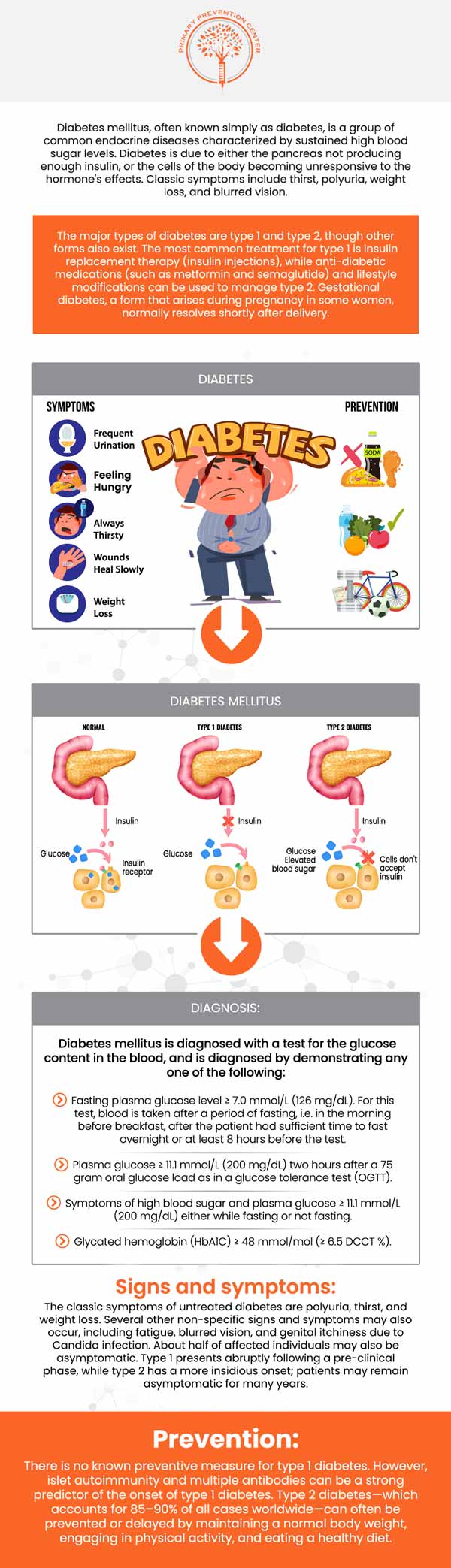
Table of Contents:
How does stress affect blood sugar levels?
Can poor sleep contribute to blood sugar imbalances?
How can sleep hygiene improve my blood sugar control?
How can I reduce stress to better manage my blood sugar?
Why Managing Stress and Sleep is Crucial for Blood Sugar Control at Primary Prevention Center
Stress triggers a number of hormonal responses that directly influence how the body manages glucose. When the body perceives stress, the adrenal glands release cortisol and adrenaline, signaling the liver to release stored glucose into the bloodstream for immediate energy. While this response can be protective in short bursts, chronic stress keeps cortisol elevated, creating persistently high blood sugar levels that can impair insulin sensitivity over time. Stress-induced glucose fluctuations are often subtle at first but can contribute to prediabetes, insulin resistance, or make existing diabetes harder to manage.
Chronic stress also influences behavior in ways that affect blood sugar. Elevated cortisol can increase appetite, drive cravings for refined carbohydrates and sugary foods, and reduce motivation for physical activity, facilitating an environment where lifestyle choices compound physiological effects. By identifying these patterns, the specialists can address both the hormonal and behavioral contributors to unstable glucose levels. Strategies often combine nutritional guidance, mindfulness, and targeted interventions to reduce the impact of stress on metabolism.
Stress impacts sleep as well, which further complicates glucose regulation. Inconsistent sleep or difficulty falling asleep elevates cortisol and disrupts other hormones like growth hormone and leptin that modulate appetite and insulin sensitivity. Chronic stress can mask underlying conditions that affect glucose management. Hidden inflammation, adrenal fatigue, and digestive imbalances can amplify the blood sugar response to stress. By using a functional, systems-oriented approach, the team at the Primary Prevention Center evaluates multiple layers of health, combining lab data, lifestyle assessment, and personalized interventions to stabilize glucose and mitigate the long-term metabolic consequences of stress.
Sleep plays a number of important roles in regulating hormones that govern glucose metabolism. Insufficient or fragmented sleep disrupts insulin sensitivity, reducing the body’s ability to move glucose into cells effectively. This can create spikes in blood sugar after meals and elevate fasting glucose in the morning, setting the stage for weight gain, insulin resistance, and difficulty managing preexisting metabolic conditions. Sleep deprivation also impacts appetite hormones, increasing ghrelin and suppressing leptin, which drives cravings for carbohydrate-rich foods. Poor sleep also impairs the nervous system’s capacity to maintain energy homeostasis. Glucose regulation relies on a delicate balance between the pancreas, liver, and peripheral tissues, and chronic sleep disruption interrupts these signaling pathways.
Inadequate sleep can lead to irregular eating patterns and reduced energy for exercise, compounding the physiological effects on blood sugar. Individuals who consistently miss restorative sleep may unknowingly create cycles where poor sleep leads to poor dietary choices and lower activity, further destabilizing glucose levels. Interventions focus on aligning sleep habits with circadian rhythms and daily routines to support long-term metabolic stability.
Chronic sleep deprivation also elevates inflammatory markers that impair insulin action and contribute to cardiovascular risk. The Primary Prevention Center specialists incorporate functional assessments, identifying both sleep disruptions and underlying health factors, and integrate lifestyle modifications that improve both sleep and blood sugar management.
Consistent sleep patterns and environmental choices can aid patients in stabilizing glucose. Providers guide patients in creating routines that reinforce circadian rhythm, such as regular sleep and wake times, reducing exposure to blue light before bed, and designing a sleep environment that promotes restorative rest. These adjustments improve insulin sensitivity, regulate appetite hormones, and reduce nighttime glucose spikes that can occur when sleep is disrupted.
Sleep hygiene also includes lifestyle factors that support metabolic efficiency. Evening routines that reduce stress, such as meditation, gentle stretching, or breathwork, lower cortisol and prepare the body for restorative sleep. Nutrition timing and light exposure are also optimized to support both sleep and blood sugar control. The Primary Prevention Center team designs these strategies in a way that reflects each individual’s schedule, stress patterns, and metabolic profile, ensuring sustainable improvements rather than temporary fixes.
Improved sleep enhances energy and consistency for other health behaviors. With stable glucose and reduced fatigue, individuals are better able to maintain regular exercise, balanced meals, and mindful eating habits, which collectively reinforce blood sugar control. Restorative sleep supports hormonal balance, reduces inflammation, and strengthens immune function, all of which enhance insulin function and protect against chronic metabolic conditions.
Addressing stress requires strategies that work on both the mind and the body. Techniques that combine behavioral, nutritional, and physiological interventions may all be considered. Mindfulness practices, meditation, and breathing exercises lower cortisol, while movement and exercise provide a physiological outlet for stress hormones. These approaches reduce the glucose spikes associated with chronic stress while enhancing overall metabolic function.
Diets that stabilize glucose, reduce inflammatory foods, and provide essential micronutrients can buffer the effects of stress on metabolism. Providers design individualized plans that consider food timing, composition, and nutrient density to reduce the impact of stress-driven cravings and glucose variability.
Lifestyle modifications extend to daily routines and sleep hygiene. Adequate rest, regular activity, and structured routines support the body’s natural rhythm, helping manage stress responses and maintain more stable blood sugar levels.
Functional assessments are used to uncover hidden contributors to stress and glucose dysregulation. Chronic inflammation, adrenal function, and digestive health are evaluated alongside psychosocial factors, creating a comprehensive plan that addresses root causes rather than treating symptoms alone. The Primary Prevention Center specialists work to empower individuals to regain control over metabolism and enhance long-term wellness.
Stress and sleep care are available at the Primary Prevention Center.
At the Primary Prevention Center, we understand the connection between stress, sleep, and blood sugar imbalances. Our holistic approach includes lifestyle changes, stress management techniques, and sleep improvement strategies to help you maintain healthy blood sugar levels. Our expert team helps you optimize both your mental and physical health to prevent blood sugar spikes and enhance overall wellness. For more information, contact us or request an appointment online. We are located at 638 Newtown-Yardley Road Suite 2G/H, Newtown, PA 18940. We serve patients from Newtown PA, Richboro PA, Newtown Grant PA, Churchville PA, Woodbourne PA, Yardley PA, Bucks County PA, and surrounding areas.
Check Out Our 5 Star Reviews



Additional Services We Offer
▸ Dietary Consultation & Planning
▸ IV Vitamin Therapy
▸ Diabetes
▸ Hypertension
▸ Insomnia
▸ Autoimmune Disease
▸ Meal planning







